What if the new $2,000 out-of-pocket cap on prescriptions actually makes your choice harder rather than easier? We know that as we move through 2026, the shift in drug costs has left the over 5,000 seniors we speak with every year feeling more confused than ever. You might worry about your trusted doctor leaving your network or feel anxious about whether your current medicare advantage plans with prescription coverage still fit your budget. It’s completely normal to feel overwhelmed. You don’t have to face this crazy maze alone.
We’ve spent 15 years helping people move from confusion to confidence by providing unbiased guidance and simplifying the jargon. By the end of this guide, you’ll know exactly how to secure an all-in-one plan that offers predictable monthly costs and protects your wallet from unexpected surprises. We’re going to walk through the 2026 network rules and the five steps to ensure your doctors and drugs are all under one roof.
Key Takeaways
- We explain why 2026 is a milestone year for bundling your hospital, medical, and drug coverage into one simple, “all-in-one” package.
- Discover how the new $2,000 out-of-pocket maximum works within medicare advantage plans with prescription coverage to help you keep more of your hard-earned money.
- We help you compare the “pay-as-you-go” savings of Part C against the fixed-cost model of Medigap to see which financial path fits your 2026 lifestyle.
- Learn why looking beyond a $0 premium is essential for your budget and how to verify that your “must-have” doctors are in your plan’s specific network.
- Use our simple 5-step process to move from confusion to confidence, ensuring you steer clear of the costly enrollment mistakes often made when calling big carriers directly.
Understanding Medicare Advantage Plans with Prescription Coverage (MAPDs) in 2026
Choosing the right healthcare shouldn’t feel like a full-time job. As we move through 2026, the “crazy maze” of the Medicare system continues to evolve, but our goal remains the same: finding a plan that protects your health and your wallet. If you’re looking for simplicity, medicare advantage plans with prescription coverage, often called MAPDs, are the primary choice for over 55 percent of Medicare beneficiaries this year. These Part C plans bundle your hospital stays, doctor visits, and pharmacy needs into one tidy package. We simplify the jargon so you know exactly how it works, moving you from a place of confusion to total confidence.
If you’re asking, What is a Medicare Advantage Plan? it’s essentially an alternative to Original Medicare provided by private companies. In 2026, these plans have become even more robust. Significant updates to the Inflation Reduction Act now mean that all MAPDs include a $2,000 annual out-of-pocket cap on prescription drugs. This change provides a level of financial security that wasn’t available just a few years ago. We are here to help you understand these shifts so you can steer clear of costly enrollment mistakes and late penalties.
The “All-in-One” Convenience Factor
The biggest draw of an MAPD is the streamlined experience. You carry one ID card in your wallet. You pay one monthly premium. You deal with one insurance carrier. This integration does more than just reduce paperwork; it improves your health. Because your medical and drug coverage live under the same roof, your plan can better coordinate care between your primary doctor and your pharmacist. This is especially vital for managing chronic conditions like diabetes or heart disease where medication timing is everything. For a deeper look at specific plan types and local options, you can explore our Medicare Advantage Guide.
MAPD vs. MA-Only: What is the Difference?
Most people need medicare advantage plans with prescription coverage, but some plans, known as MA-Only plans, exclude drugs. Why would anyone choose that? Usually, it’s for veterans who get their medications through the VA or individuals with other “creditable” coverage. If you don’t have a valid reason for skipping drug coverage, you face two major risks. First, you’ll pay for every pill out of pocket. Second, you’ll likely face a permanent late enrollment penalty if you try to add drug coverage later. We usually recommend integrated coverage for our clients to ensure they are protected from day one.
How Drug Coverage Works Within a 2026 Part C Plan
Managing your health shouldn’t feel like a full-time job. In 2026, medicare advantage plans with prescription coverage combine your doctor visits and your pharmacy needs into one simple package. This integrated approach is a big reason why recent enrollment trends show more seniors choosing these plans every year. We help you look past the marketing brochures to see how these plans actually pay for your medications at the counter.
The New 2026 Out-of-Pocket Drug Cap
The $2,000 cap is the most significant pharmacy benefit change in decades. This new limit means that once you spend $2,000 on your covered prescriptions in 2026, you won’t pay another penny for your drugs for the rest of the calendar year. It protects you from the catastrophic costs that used to burden families who needed expensive specialty medications. This safety net makes Medicare Advantage even more attractive for 2026 because your financial risk is finally capped at a predictable, manageable number.
Formularies and Pharmacy Networks
Every plan uses a “formulary,” which is a list of covered drugs grouped into tiers. Tier 1 usually includes preferred generics with the lowest co-pays, while Tier 5 covers specialty drugs for complex conditions. Where you shop matters just as much as what you take. Most medicare advantage plans with prescription coverage use “Preferred” pharmacies where your costs are much lower than at “Standard” locations. We often suggest mail-order options, which can save you a trip to the store and typically offer a 90-day supply for a lower total cost. If you feel stuck, you can view our guide on drug tiers to see where your medications land.
Plans also use tools like Step Therapy and Prior Authorization to manage costs. Step therapy requires you to try a lower-cost, effective drug before the plan covers a more expensive brand-name version. Prior authorization means your doctor must provide extra paperwork to prove a specific medication is medically necessary before the plan agrees to pay. Because these rules and drug lists change every January 1st, we use our professional tools to verify your specific medications against 40+ carrier lists every year. Our mission is to remove the anxiety from this process, so if you want to verify your pharmacy network, you can schedule a quick call with us to get the facts.
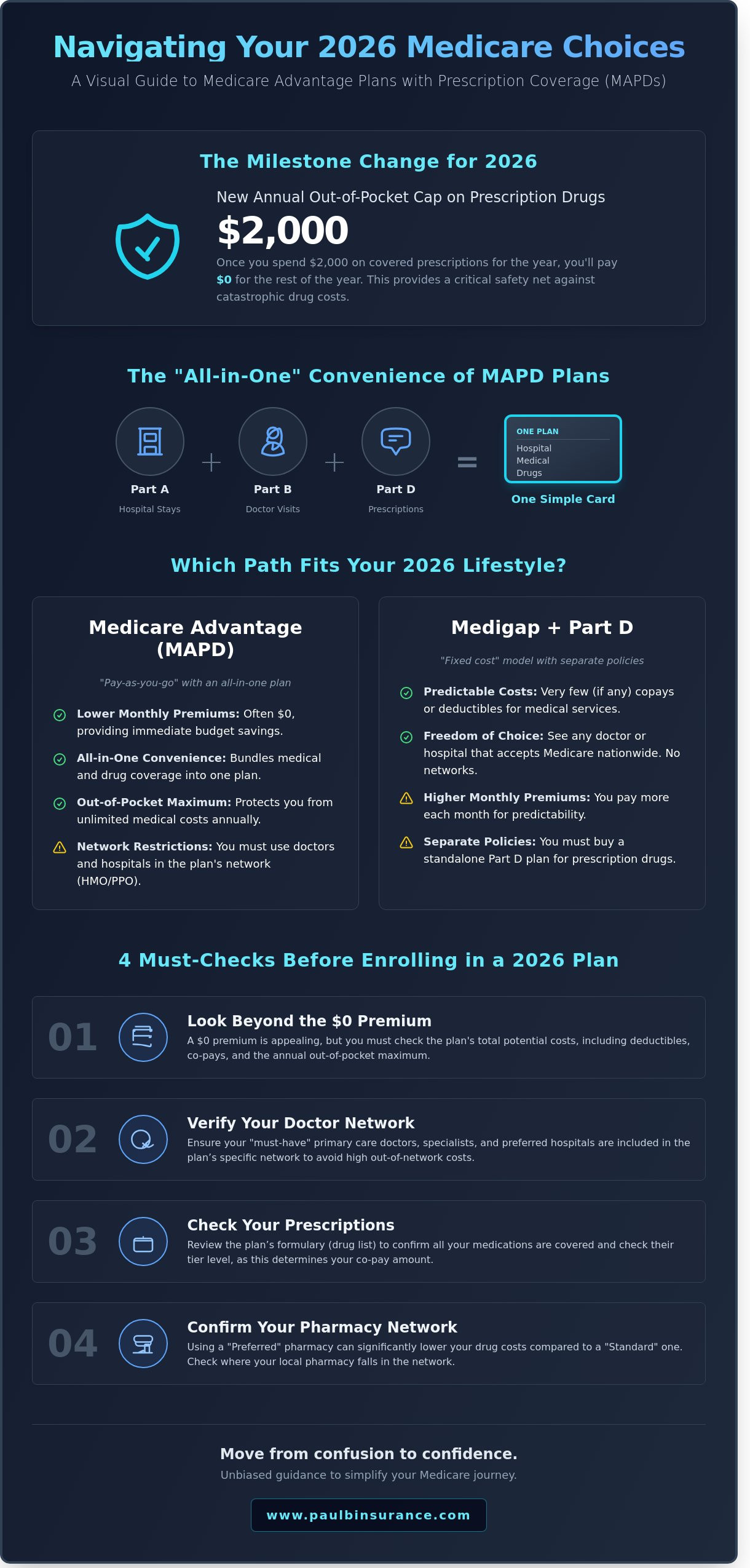
MAPD vs. Medigap with Part D: Which Path is Right for You?
Choosing between medicare advantage plans with prescription coverage and a Medigap plan is one of the most important steps in your 2026 health journey. We see many seniors feel torn between these two paths. It helps to think of it as a choice between a “pay-as-you-go” model and a “fixed-cost” model. MAPD plans usually have lower monthly premiums, often starting at $0, while Medigap plans have higher monthly costs but offer more predictable expenses when you actually use medical services.
Your lifestyle plays a huge role here. If you plan to spend 2026 traveling across state lines, a Medigap plan might be your best bet. It allows you to see any doctor in the country who accepts Medicare. You can learn more about this in our Medigap overview. However, if you prefer having all your benefits in one place, an MAPD plan simplifies things. For a deeper look at how these bundled options work, the official CMS guide on Understanding Medicare Advantage Plans provides a great foundation for your research.
When to Choose a Medicare Advantage Prescription Drug Plan
We often recommend medicare advantage plans with prescription coverage for those who want to maximize their monthly budget. In 2026, many of these plans offer extra perks that Original Medicare simply doesn’t cover. This includes things like fitness memberships, meal delivery after a hospital stay, and transportation to appointments. These plans are also famous for bundling dental, vision, and hearing benefits directly into the package. While these bundles are helpful, some clients find they need more comprehensive care, which is why we also offer specialized dental insurance options to fill any remaining gaps.
When Standalone Part D is the Better Move
There are times when keeping your drug coverage separate is the smarter strategy. If you have a specific, rare medication, you might need a standalone Medicare Part D plan that has that exact drug on its list of covered medicines. By pairing a standalone drug plan with a Medigap policy, you gain the ultimate freedom to choose your doctors. You aren’t restricted by a network. This is a common choice for those who want to avoid the “prior authorization” hurdles that sometimes come with Advantage plans. It ensures your healthcare stays between you and your doctor, with no middleman involved.
Evaluating 2026 Plans: 4 Things You Must Check Before Enrolling
Choosing medicare advantage plans with prescription coverage shouldn’t feel like a high-stakes guessing game. We know your mailbox is likely overflowing with glossy brochures promising the world for $0. Our job is to help you look past the marketing and focus on the facts. We focus on four critical areas: the total cost of care, doctor networks, star ratings, and the fine print in the Evidence of Coverage. We simplify the jargon so you know exactly how your plan works before you sign anything.
- 2026 Star Ratings: These 1 to 5 star scores are updated every October. They tell us if a plan has a history of pharmacy errors or poor customer service. We only recommend plans that prove they can take care of you.
- Provider Networks: A doctor you’ve seen for ten years might leave a network on January 1st. We verify your “must-have” specialists for the 2026 plan year so you don’t lose access to the care you trust.
- The Evidence of Coverage (EOC): This document is often over 100 pages long. It’s enough to give anyone a headache. We read the fine print for you to identify changes in co-pays or hidden requirements for prior authorizations.
The Total Cost of Care Calculation
A $0 monthly premium is attractive, but it’s only one piece of the puzzle. We look at the “Total Cost of Care,” which adds up your premiums, your specific deductibles, and the estimated co-pays for every medication you take. For 2026, the $2,000 out-of-pocket cap on prescription drugs serves as a massive safety net. If your drug costs reach that $2,000 limit, you’ll pay $0 for covered medications for the rest of the year. We do this math for you so you can sleep better knowing your budget is protected.
Network Stability and Specialty Drugs
Drug formularies change every year. A medication that was affordable in 2025 might move to a higher “Specialty” tier in 2026, which can drastically increase your costs. This happens often with biologics or cancer treatments. We monitor these shifts across 40+ different carriers to ensure your medications remain accessible. As independent brokers, we advocate for you, not the insurance company. We help you move from confusion to confidence by finding the plan that treats your specialty drugs fairly.
Ready to see how these 2026 changes affect your specific medications? Read our full Medicare Advantage guide to find the right fit for your needs.
How The Modern Medicare Agency Simplifies Your Choice
We know that 2026 brings new changes to out-of-pocket drug caps and plan structures. It is easy to feel overwhelmed by the stacks of mail piling up on your kitchen counter. Our team at The Modern Medicare Agency acts as your personal shield against the noise. We move you from confusion to confidence by handling the heavy lifting of research and comparison. Finding the right medicare advantage plans with prescription coverage should not feel like a second job. We simplify the jargon so you know exactly how your plan works before you ever sign a document.
40+ Carriers, One Unbiased Goal
A “captive” agent works for one specific insurance company. They are required to sell you that company’s products, even if a better or more affordable option exists down the street. We do things differently. As independent brokers, we shop over 40 different carriers to find your perfect match. Our loyalty stays with you, not the insurance giants. Our service costs you nothing. The carriers pay us a standard fee, which means you get expert guidance without a single added expense. We work for you to ensure your doctors and pharmacies remain in-network for the coming year.
Our 5-step process is designed to remove anxiety from the equation:
- Listen: We start by understanding your unique health needs and budget goals.
- Analyze: We check your specific medications against 2026 formularies to find the lowest costs.
- Compare: We present the top three options side-by-side so you can see the real differences.
- Enroll: We manage the paperwork and digital filings to ensure a 100% accurate enrollment.
- Support: We provide year-round advocacy. If a bill looks wrong in July, you call us, not the carrier.
Your Next Steps for 2026
The Annual Enrollment Period (AEP) begins on October 15 and ends on December 7. To prepare for a smooth transition, we recommend gathering your current list of medications and the names of your primary specialists. This allows us to run a real-time analysis of which medicare advantage plans with prescription coverage provide the best value for your specific health profile. You can learn more about these options in our medicare advantage guide.
We invite you to schedule a “No-Pressure” call with Paul and our team for your 2026 planning. We promise a calm, patient conversation where you are never rushed and never pressured. We are here to protect your health and your wallet. Let us help you start the new year with the peace of mind you deserve.
Take Control of Your 2026 Medicare Journey
Navigating the 2026 healthcare landscape requires a clear understanding of how your drug costs and medical benefits fit together. We’ve explored the critical differences between integrated plans and Medigap options; we also highlighted the four essential checks you must perform to avoid enrollment penalties this year. Finding the right medicare advantage plans with prescription coverage shouldn’t feel like a guessing game. It’s about matching your specific prescriptions to the right 2026 formulary so you don’t overpay at the pharmacy counter.
We’re here to simplify the jargon and protect you from costly mistakes. Our team provides licensed expertise in 34 states and represents over 40 top-rated carriers to ensure you have every option available. You’ll receive patient, expert guidance that’s never rushed and never pressured. We’re dedicated to helping you move from a state of confusion to complete confidence. Your health and budget deserve a plan that works as hard as you do. Schedule a Call With Paul to Find Your 2026 Plan today. We look forward to helping you secure the peace of mind you deserve for the year ahead.
Frequently Asked Questions
Do all Medicare Advantage plans include prescription drug coverage?
No, not every plan includes this specific benefit. While 89% of Medicare Advantage plans offered in 2026 come with built-in drug coverage, some specialized options like Medical Savings Accounts require you to look elsewhere. If you choose a plan without it, you might face a late enrollment penalty later. We help you check the summary of benefits so you don’t accidentally pick a plan that leaves your pharmacy costs unprotected.
What happens to the “Donut Hole” in 2026?
The “Donut Hole” is officially a thing of the past as of January 2025. In 2026, you’ll benefit from a simplified structure where you never pay more than $2,000 out of pocket for covered drugs. This change removes the old coverage gap that used to cause so much stress for seniors. Once you hit that $2,000 limit, your plan pays 100% of your covered drug costs for the rest of the year.
Can I add a standalone Part D plan to my Medicare Advantage plan?
No, you usually can’t have both at the same time. If you try to join a standalone Part D plan while enrolled in medicare advantage plans with prescription coverage, Medicare will likely drop you from your Advantage plan. This is a common mistake that can lead to losing your dental or vision benefits. We make sure you choose the right all-in-one plan from the start to avoid this confusion.
How much will I pay for drugs in 2026 if I reach the $2,000 cap?
You’ll pay $0 for your covered prescriptions for the remainder of the calendar year once you reach the $2,000 cap. This $2,000 limit applies to your actual out of pocket spending, not the total retail cost of the medication. It’s a massive relief for the 1 in 4 seniors who previously spent much more. You can also use the Medicare Prescription Payment Plan to spread these costs into monthly installments throughout 2026.
Are insulin costs still capped in 2026 Medicare Advantage plans?
Yes, your insulin costs remain capped at a maximum of $35 for a one month supply. This protection applies even if you haven’t met your yearly deductible yet. Since this law took effect, it has saved millions of Americans an average of $440 per year. We’ll verify that your specific brand of insulin is on your plan’s list so you get this guaranteed pricing without any surprises or hidden pharmacy fees.
What if my drug isn’t on my plan’s formulary?
You can request a “formulary exception” if your specific medication isn’t on the approved list. Your doctor must provide a statement explaining why the drug is medically necessary for your health. If you’re new to a plan, you’re often entitled to a one time, 30 day transition fill. This gives us time to work together on an appeal or find a similar medication that your plan covers fully at a lower tier.
Can I change my MAPD plan if my prescriptions change mid-year?
You generally can’t switch plans mid-year just because your prescriptions changed. Most people must wait for the Annual Enrollment Period that starts October 15. However, you might qualify for a Special Enrollment Period if you move to a new zip code or qualify for “Extra Help.” About 13 million people currently use Extra Help to lower their costs and gain more flexibility with plan changes throughout the year.
Is there a penalty if I wait to join a plan with drug coverage?
Yes, you’ll likely face a permanent late enrollment penalty if you go 63 days or more without creditable coverage. This penalty adds 1% of the national base beneficiary premium to your monthly bill for every month you were eligible but didn’t enroll. In 2026, that base premium is $35.00. We’ll help you secure a plan now so you don’t get stuck with these extra costs for the rest of your life.






