If a Medicare Advantage plan costs $0 per month, why did the maximum out-of-pocket limit for some beneficiaries reach as high as $9,350 in 2025? It feels like a trap when a plan that promised to save you money suddenly hits you with a $350 daily hospital copay or a 20% coinsurance bill for specialized treatment. You’ve likely felt that familiar knot in your stomach while trying to figure out what are the hidden costs of medicare advantage plans before the 2026 enrollment season begins. It’s exhausting to feel like you’re staring at a maze of fine print while your financial security hangs in the balance.
We believe you deserve total clarity, not a sales pitch. We’re pulling back the curtain on those “zero-dollar” premiums to show you exactly how these plans function so you can build a predictable monthly budget. You’ll learn the difference between fixed copays and unpredictable coinsurance, how network changes impact your bottom line, and how to spot the five most common financial surprises before they happen. This guide moves you from confusion to confidence, ensuring you choose a plan that protects your health and your hard-earned savings in 2026.
Key Takeaways
- Understand why a “$0 premium” doesn’t mean free coverage and how to properly budget for your mandatory Medicare Part B monthly costs.
- Protect your savings by learning how to identify the 2026 Maximum Out-of-Pocket (MOOP) limits and the impact of coinsurance on your budget.
- Discover what are the hidden costs of medicare advantage plans regarding restrictive provider networks and the potential care delays caused by prior authorizations.
- Learn a simple two-step method to audit your prescriptions and doctor visits so you can estimate your total annual healthcare spending with clarity.
- Move from confusion to confidence by seeing how an independent expert provides the unbiased guidance needed to choose a plan that truly protects your health and wealth.
The “$0 Premium” Mirage: Understanding the Real Price of Admission
Medicare Advantage television commercials are everywhere. They promise $0 premiums and “money back in your Social Security check.” It sounds like a dream. For many seniors, this leads to a “mirage” where the real price of admission stays hidden behind flashy marketing. We want to help you move from confusion to confidence by pulling back the curtain on these costs. We simplify the jargon so you know exactly how it works before you sign on the dotted line.
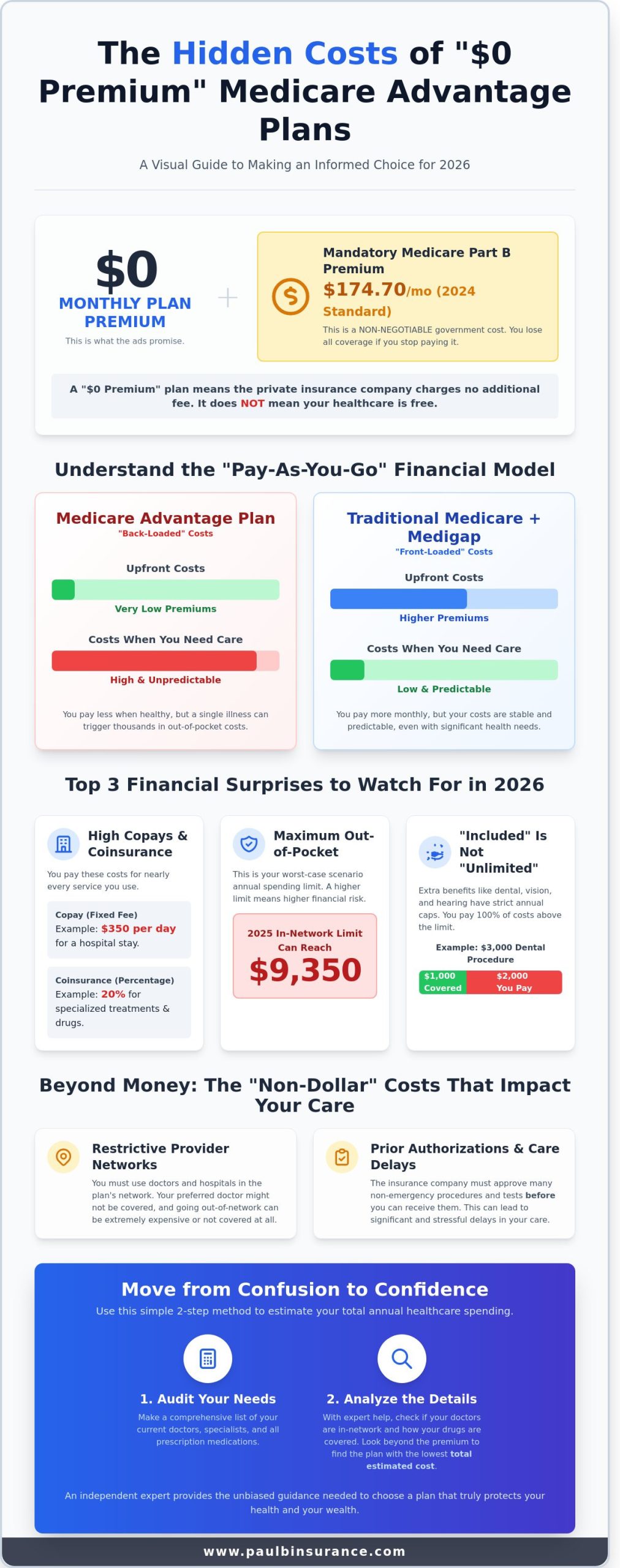
First, let’s clear up a common misunderstanding. A $0 premium does not mean your health insurance is free. It simply means the private insurance company is not charging you an additional monthly fee on top of what you already pay the government. To stay enrolled in any Medicare Advantage program, you must continue paying your Medicare Part B premium. In 2024, the standard monthly premium for Part B is $174.70. If you stop paying this, you lose your coverage. When you ask what are the hidden costs of medicare advantage plans, the Part B premium is the very first “hidden” cost because people assume $0 means $0 total.
Medicare Advantage (Part C) operates on a “pay-as-you-go” model. While Traditional Medicare with a Medigap plan has higher upfront monthly costs, Advantage plans are “back-loaded.” This means you pay less when you are healthy and more when you actually need medical care. You might save money on premiums today, but a single hospital stay could trigger thousands of dollars in copays. Our goal is to ensure you steer clear of costly enrollment mistakes by looking at the total annual cost, not just the monthly bill.
How Private Insurers Offer $0 Premiums
The government pays private insurers a set amount of money for every person they enroll. This is a rebate system. If the insurer manages your care for less than what the government pays them, they use the “extra” money to offer $0 premiums or extra perks. By 2026, new regulations will change how these rebates are calculated. This shift could mean insurers have less “extra” money. You may see higher out-of-pocket maximums or reduced benefit limits as companies adjust to these 2026 funding changes. We provide unbiased guidance to help you see how these shifts affect your specific zip code.
The Distinction Between “Free” and “Included”
Television commercials use an emotional “hook” to make you feel like you’re missing out on free money. There is a big difference between a service being “free” and being “included.” Extra benefits like dental, vision, and hearing usually have strict internal limits. For example, a plan might offer “included” dental care but cap the benefit at $1,000 per year. If you need a $3,000 procedure, you are responsible for the balance. Understanding what are the hidden costs of medicare advantage plans requires looking past the “included” label to find the actual dollar limits. We are here to protect and empower you, making sure you feel never rushed and never pressured while comparing these details.
Our 5-step process takes you from a state of being overwhelmed to a state of total clarity. We act as your advocate, not a salesperson. When you work with an independent broker, you gain options. When you work with a captive agent, you lose them. Let us help you find the path from confusion to confidence.
Beyond the Premium: Copayments, Coinsurance, and the MOOP Limit
You might see a $0 premium and think your healthcare is free. That’s a common misunderstanding that leads many seniors to feel overwhelmed when the bills actually arrive. When people ask what are the hidden costs of medicare advantage plans, they are often looking at the monthly premium while ignoring the daily reality of usage. To find peace of mind, you have to look at the three pillars of plan spending: copayments, coinsurance, and the Maximum Out-of-Pocket (MOOP) limit.
Copayments are fixed dollar amounts you pay for specific services. You might pay $0 for a primary care visit but $40 for a specialist. Coinsurance is more unpredictable because it’s a percentage of the total cost. For example, many plans charge a 20% coinsurance for Part B drugs or durable medical equipment. If you require chemotherapy, dialysis, or specialized imaging like an MRI, these costs can escalate quickly. High-cost triggers like these represent what are the hidden costs of medicare advantage plans that catch many retirees off guard. We simplify the jargon so you know exactly how these numbers affect your bank account.
The MOOP is your financial safety net for the year. It’s the absolute maximum you’ll pay for covered medical services. Once you reach this limit, the plan pays 100% for the remainder of the year. While it sounds high, it protects you from total financial ruin during a health crisis. You can compare these limits against the official Medicare costs to see how Advantage plans differ from Original Medicare.
The 2026 Out-of-Pocket Max: What It Covers (and What It Doesn’t)
For 2026, the maximum in-network MOOP is expected to be $9,350 or higher, though many plans set their limits lower to stay competitive. This limit only applies to Medicare Part A and Part B services. It’s vital to remember that your Part D prescription drug costs do not count toward this medical MOOP. They have their own separate spending limits. If you’re feeling confused about which plans offer the best protection, our comprehensive Medicare Advantage guide provides a clear comparison of current options.
Hospitalization and Skilled Nursing Surprises
Hospital stays often involve “per-day” copays rather than a single flat fee. A plan might charge you $350 per day for the first five days. If you’re hospitalized for a week, that’s a $1,750 bill you didn’t see coming. Skilled nursing care follows a different pattern. Most plans cover the first 20 days at no cost, but on day 21, you could face a daily co-pay exceeding $200. A Skilled Nursing Facility is a post-hospitalization recovery center where you receive professional medical care and rehabilitation services. Knowing these timelines helps you move from confusion to confidence.
The maze of Medicare doesn’t have to be stressful. If you want to steer clear of costly enrollment mistakes, you can schedule a call with Paul to get unbiased, expert guidance tailored to your specific needs.
The “Non-Dollar” Costs: Networks, Prior Authorizations, and Plan Stability
You deserve to feel confident and secure in your healthcare choices. When people ask what are the hidden costs of medicare advantage plans, they usually focus on the deductibles or the copays. However, some of the most significant costs don’t show up on a monthly bill. They’re found in the time you spend waiting for approvals, the stress of losing a trusted doctor, and the miles you drive to find a facility that’s actually in your network. These “non-dollar” costs can impact your quality of life just as much as a high premium.
The Price of Provider Restrictions
In an HMO model, you’re typically required to choose a primary care doctor who acts as a gatekeeper. If you need to see a specialist, you must get a referral first. This adds a layer of administrative friction that can delay your care by weeks. If your favorite specialist decides to leave the plan network on January 1, 2026, you’re often left with two difficult choices: find a new doctor you don’t know or pay the full cost of the visit out of your own pocket. For the 20% of beneficiaries living in rural areas, these restrictions are even more taxing. You might find that the only “in-network” specialist is located 50 miles away, adding the cost of gas, hotel stays, and physical exhaustion to your medical journey. This is a major departure from Traditional Medicare, where 99% of doctors and hospitals across the country accept your coverage without any network hurdles. You can review the official Medicare cost breakdown to see how these structures differ from the standard Part B framework.
Prior Authorization: The Hidden Hurdle
Prior authorization is essentially the insurance company’s way of giving a “second opinion” on your doctor’s orders before they agree to pay for a service. It’s one of the most common answers to the question of what are the hidden costs of medicare advantage plans because it places the burden of proof on the patient. In 2021, data showed that Medicare Advantage plans issued over 35 million prior authorization requests. While these are intended to manage costs, they frequently lead to denied care or dangerous delays in treatment. For 2026, there’s a bit of relief on the horizon. New “Gold Carding” rules from CMS require plans to respond to urgent requests within 72 hours and standard requests within seven days. While this move toward “From Confusion to Confidence” is helpful, the hurdle still exists. You’re still asking a corporation for permission to follow your doctor’s advice.
Plan instability is another factor that often catches seniors off guard. Medicare Advantage plans operate on one-year contracts with the federal government. This means the benefits you enjoy in 2026 aren’t guaranteed for 2027. Insurers can change their drug lists, increase your maximum out-of-pocket limit, or even pull out of your zip code entirely. In 2024, several major carriers announced they’d reduce “extra” benefits to protect their profit margins. This annual “plan churn” forces you to re-evaluate your entire healthcare strategy every October. It turns what should be a peaceful retirement into a recurring cycle of paperwork and anxiety. We believe your coverage should be a source of peace, not a source of constant homework.
How to Calculate Your Total Cost of Care for 2026
Calculating your total cost of care for 2026 doesn’t have to be a headache. You can move from confusion to confidence by following a simple, logical process that looks beyond the $0 monthly premium. We simplify the jargon so you know exactly how the numbers work for your specific health situation.
First, audit your current prescriptions and check them against the 2026 formulary. Drug lists change every year on January 1. A medication that cost $20 last year might move to a higher tier with a $45 copay in 2026. Use your actual medication list to see how these shifts impact your wallet.
Next, estimate your utilization rate. Look at your calendar from the last 12 months. If you saw a specialist six times and had three lab tests, use those numbers to project your 2026 costs. If a specialist copay is $40, that is $240 right there. Identifying what are the hidden costs of medicare advantage plans starts with a clear look at your actual medical usage rather than best-case scenarios.
Third, factor in the limits on extra benefits. Many plans advertise “free” dental or vision, but these often have a hard cap, such as $1,000 or $1,500 per year. If you need a $2,500 dental bridge, you’ll be responsible for the remaining $1,000 out of pocket. This is one of the most common ways people discover what are the hidden costs of medicare advantage plans after it’s too late to switch for the year.
Finally, compare your estimated total to a Medigap plan premium. While Medigap has a higher monthly bill, it removes the guesswork of copays and coinsurance.
Advantage vs. Medigap: The Financial Math
Medigap is a front-loaded financial strategy. You pay a predictable monthly premium, but you often pay $0 when you actually walk into the doctor’s office. This makes it the safer choice for people with chronic conditions or those who want a fixed budget. Healthy individuals who rarely see a doctor might save money with Advantage in the short term, but a single unexpected surgery can quickly trigger the $5,000 to $9,000 out-of-pocket maximum. Medigap provides a fixed monthly budget for peace of mind while Advantage offers lower monthly costs with variable copays.
The Impact of the 2026 Part D Changes
The landscape of Medicare Part D changes significantly in 2026 due to the $2,000 out-of-pocket cap. This federal limit means once you spend $2,000 on covered prescriptions, your plan pays 100 percent of your drug costs for the rest of the year. This cap makes Advantage plans much more attractive for users with high-cost specialty drugs who previously faced unlimited costs in the “donut hole.” Starting in 2025 and continuing through 2026, you also have the “M3” option, known as the Medicare Prescription Payment Plan. This allows you to spread your drug costs into monthly installments rather than paying a huge sum at the pharmacy counter in January.
Stop guessing about your 2026 healthcare costs and get a personalized plan today. Schedule a Call With Paul to find the clarity you deserve.
Moving from Confusion to Confidence: How We Help You Uncover the Truth
The 2026 Medicare landscape feels more like a puzzle than a healthcare system. You might feel overwhelmed by the constant mailers and conflicting advice. We are here to stop the noise. As independent brokers, we represent over 40 different insurance carriers. This independence is your greatest asset because we don’t have a quota to fill for a specific brand. Our only loyalty is to you and your bank account. We provide unbiased guidance designed to replace your stress with a sense of total security.
Our approach is simple. We work for you, not the insurance companies. We translate the complex jargon into plain English so you know exactly how your coverage functions. You deserve to know the truth about your benefits. We help you steer clear of costly enrollment mistakes and late penalties that can haunt your finances for years. Our mission is to move you from a state of confusion to a place of absolute confidence.
Why an Independent Broker is Your Best Defense
There is a massive difference between a captive agent and an independent broker. A captive agent works for one specific company and can only offer you that company’s products. If that plan isn’t a good fit, they can’t tell you to go elsewhere. We are different. We use professional analytical software to run “Total Cost” comparisons across the entire 2026 market. This software allows us to calculate your projected annual spend, including every copay and prescription cost. This is the only way to truly see what are the hidden costs of medicare advantage plans before you enroll. Best of all, our expert services are provided at $0 cost to you. The insurance carriers pay us, but you get the benefit of our full market research.
- Step 1: The Discovery Conversation. We listen to your concerns and identify your specific health priorities for 2026.
- Step 2: Information Gathering. You provide your list of doctors, preferred hospitals, and current medications.
- Step 3: Comprehensive Market Scan. We use our technology to filter through 40+ carriers to find the top three matches.
- Step 4: The Comparison Review. We sit down together to look at the numbers, highlighting what are the hidden costs of medicare advantage plans that others might miss.
- Step 5: Stress-Free Enrollment. We handle all the paperwork and follow up to ensure your new ID cards arrive on time.
Our commitment to you doesn’t end on January 1st. We provide year-round support to every client we serve. If you receive a medical bill that doesn’t look right in the middle of July, you call us. If your primary doctor leaves the network in September, we help you find a new one or plan for the next enrollment period. You are never alone in this process; we are your advocates for the life of your policy.
Your Next Steps for a Stress-Free 2026
Preparation is the enemy of anxiety. To get started, gather a complete list of your current specialists and the exact dosages of your medications. Having this data ready makes our analysis much faster and more accurate. You don’t have to navigate this crazy maze by yourself. We have the tools, the experience, and the patience to ensure you get the coverage you actually need. Take the first step toward peace of mind right now. Schedule a free, no-pressure consultation with our team today.
Take Control of Your 2026 Healthcare Future
Navigating the 2026 healthcare landscape requires more than just looking at a $0 monthly premium. You now understand what are the hidden costs of medicare advantage plans, from high Maximum Out-of-Pocket limits to the restrictive networks that can dictate your choice of doctor. These expenses often hide in plain sight. They wait until you need care to impact your bank account. By calculating your total cost of care today, you avoid the stress of unexpected medical bills later.
You don’t have to face these complex decisions alone. I provide independent access to over 40 top-rated insurance carriers across more than 34 states. This ensures you receive unbiased guidance tailored to your specific health needs and budget. My “Never Rushed, Never Pressured” guarantee means we’ll take the time to simplify every detail until you feel completely secure in your choice. We’ll turn that mountain of paperwork into a clear, manageable path forward.
From Confusion to Confidence: Schedule Your 2026 Medicare Review with Paul
It’s time to replace your worry with a solid plan that protects both your health and your hard-earned savings. You deserve to move into the new year with total peace of mind.
Frequently Asked Questions
Is Medicare Advantage really “free” if it has a $0 premium?
No, a $0 premium plan isn’t actually free because you still must pay your monthly Medicare Part B premium, which is $174.70 in 2024. You also face pay as you go costs like a $45 copay for a specialist visit or 20% for chemotherapy. These out-of-pocket expenses are the real what are the hidden costs of medicare advantage plans that can surprise you during a health crisis.
Can a Medicare Advantage plan change its costs in the middle of the year?
Your plan cannot change its premium or deductible mid-year, but your costs can still shift if your doctor leaves the network. Insurance companies can also change their list of covered drugs, known as a formulary, every 30 days. If your $20 medication is moved to a higher tier, your cost could jump to $47 or more without warning before the year ends.
What happens to my costs if I see a doctor who is out-of-network?
If you have an HMO plan, you’ll likely pay 100% of the bill for seeing an out-of-network doctor, except in an emergency. PPO plans allow out-of-network care, but your coinsurance often jumps from a $20 copay to 40% or 50% of the total cost. This means a $1,000 procedure could cost you $500 out of pocket just for choosing the wrong provider.
Does the 2026 $2,000 drug cap apply to Medicare Advantage plans?
Yes, the $2,000 out-of-pocket cap for prescription drugs applies to all Medicare Advantage plans with drug coverage starting in 2025 and continuing into 2026. This federal limit, established by the Inflation Reduction Act, protects you from unlimited spending on medications. Once you hit that $2,000 mark, you pay $0 for your covered Part D drugs for the rest of the calendar year.
Why do some doctors refuse to accept Medicare Advantage plans?
Many doctors opt out because Medicare Advantage plans often pay lower reimbursement rates and require prior authorization for basic procedures. A 2023 survey found that 13% of physicians don’t accept these plans because of the administrative burden. This creates a hidden hurdle where you might have the insurance, but your preferred specialist at a top hospital won’t take your specific plan.
How much should I keep in savings to cover my Medicare Advantage MOOP?
You should keep at least $9,350 in an emergency fund to cover the maximum out-of-pocket limit allowed by law in 2025. While the average limit is closer to $5,000, a serious illness could force you to pay the full legal amount in a single year. Understanding what are the hidden costs of medicare advantage plans means preparing for this scenario so a hospital stay doesn’t ruin your retirement.
Can I switch from Medicare Advantage back to Medigap if the costs are too high?
You can switch during the Annual Enrollment Period, but you’ll likely have to pass a medical background check to get a Medigap policy. In 46 states, private insurers can deny you coverage or charge higher rates if you have pre-existing conditions like diabetes or heart disease. This makes the initial choice critical, as you aren’t guaranteed a way back to Original Medicare without financial penalties.