Is your mailbox overflowing? Are you tired of the confusing calls and complicated terms? Navigating the world of medicare advantage plans can feel overwhelming, leaving you worried about making a costly mistake or losing access to your trusted doctor. It’s a heavy weight to carry when all you truly want is simple, clear guidance and peace of mind for your health.
You are not alone in feeling this way, and we are here to help. This guide was created to be your trusted resource, cutting through the noise and sales pressure. We believe that understanding your healthcare options shouldn’t be a stressful experience. It should be an empowering one.
We promise to walk you through everything you need to know in simple, straightforward language. From how these plans work to comparing your specific options, our goal is to help you move from a state of confusion to one of complete confidence in your healthcare decisions.
Key Takeaways
- Understand the fundamental difference between Original Medicare and choosing a bundled, ‘all-in-one’ private plan.
- Learn how different types of medicare advantage plans can affect your choice of doctors, referral requirements, and total out-of-pocket costs.
- Weigh the key pros and cons to confidently determine if an Advantage plan is the right fit for your specific health and budget needs.
- Discover the critical enrollment periods to avoid costly penalties and ensure you don’t miss your window to join or switch plans.
What Is a Medicare Advantage Plan (Part C)?
Navigating your Medicare options can feel overwhelming, but it doesn’t have to be. Let’s simplify one of the most common choices you’ll face.
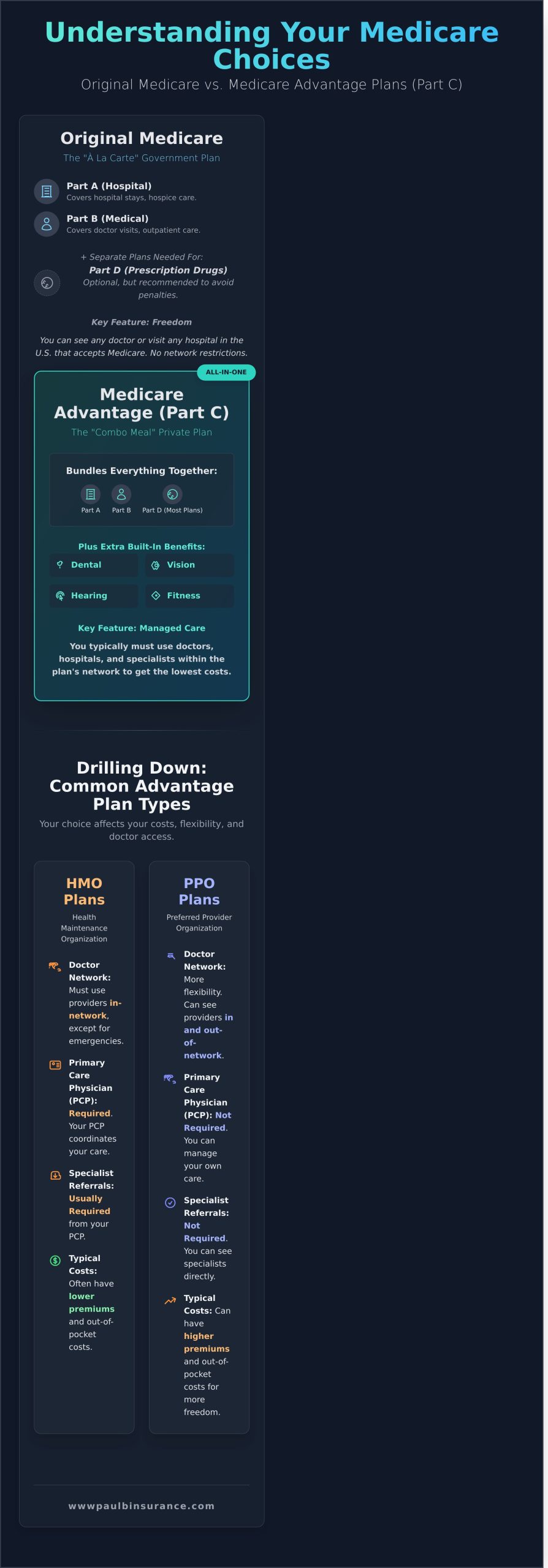
Think of Original Medicare (Part A and Part B) as ordering your healthcare “à la carte.” You get hospital coverage here, doctor coverage there. A Medicare Advantage Plan, also known as Part C, is like ordering a “combo meal.” It’s an all-in-one alternative to Original Medicare, bundling your benefits into a single, convenient plan.
These plans are offered by private insurance companies that are approved by Medicare. While the structure is different, every Medicare Advantage plan is required by law to cover everything that Original Medicare covers. The core trade-off is that you typically receive care from a network of doctors and hospitals in exchange for extra benefits and often, a lower overall cost.
How Advantage Plans Work with Original Medicare
It’s a common point of confusion, so let’s make it simple. When you enroll in a Part C plan, you are still in the Medicare program and must continue to pay your monthly Part B premium. However, the private insurance company takes over the administration of your benefits. You’ll receive a new ID card from them, which you’ll use for all your medical services instead of your red, white, and blue Medicare card.
What Do These Plans Typically Include?
One of the main draws of an Advantage Plan is the convenience of having your benefits bundled together. Most plans include:
- Part A Coverage: For hospital stays, skilled nursing facility care, and hospice.
- Part B Coverage: For doctor visits, outpatient care, and preventive services.
- Part D Coverage: Most plans include prescription drug coverage, so you don’t need a separate plan.
- Extra Benefits: This is where plans really differ. Many offer routine dental, vision, and hearing coverage, plus perks like fitness memberships (e.g., SilverSneakers).
Who Offers Medicare Advantage Plans?
You’ve likely seen the names on TV or in your mailbox: companies like Humana, Aetna, and UnitedHealthcare are major providers of medicare advantage plans. But here’s the crucial part: plans are not one-size-fits-all. The benefits, costs, and network of doctors can change significantly from one county to the next. That’s why comparing your local options is not just a good idea-it’s essential to finding the coverage that truly serves your needs with confidence.
The Different Types of Medicare Advantage Plans Explained
Navigating the world of Medicare can feel like learning a new language, especially with all the acronyms like HMO and PPO. But don’t worry-we’re here to make it simple. Think of these plan types not as confusing labels, but as different paths to getting the healthcare you need. The right path for you depends on what you value most: cost, flexibility, or a combination of both.
The main differences come down to three simple things: which doctors you can see (your network), whether you need a referral for specialists, and how much you’ll pay out-of-pocket.
HMO (Health Maintenance Organization) Plans
HMO plans are often a great choice if you’re looking for predictable costs and coordinated care. With an HMO, you choose a Primary Care Physician (PCP) from within the plan’s network. Your PCP is your trusted guide, managing your care and providing referrals when you need to see a specialist. Because care is kept within a specific network of doctors and hospitals, HMOs can typically offer lower monthly premiums and out-of-pocket costs.
PPO (Preferred Provider Organization) Plans
If freedom and flexibility are your top priorities, a PPO plan might be the perfect fit. PPO plans give you the choice to see providers both in and out-of-network. While you’ll always save money by staying in-network, you have the freedom to see any doctor who accepts the plan. Plus, you don’t need to select a PCP or get a referral to see a specialist, giving you direct access to the care you need.
Other Common Plan Types: SNP and PFFS
While HMOs and PPOs are the most common, there are other medicare advantage plans designed for unique situations. Special Needs Plans (SNPs) are tailored for individuals with specific chronic conditions (like diabetes) or those who qualify for both Medicare and Medicaid. Private Fee-for-Service (PFFS) plans are less common but offer flexibility, as long as your doctor agrees to the plan’s payment terms for each service.
So, which type is best? The honest answer is: it depends entirely on you. Understanding these core differences is the most important step toward choosing with confidence. As you weigh these options, independent resources like Forbes’ analysis of top plans can also help you see how different insurance carriers measure up. The goal is to find a plan that fits your health needs, your budget, and your lifestyle, giving you true peace of mind.
Pros and Cons: Is a Medicare Advantage Plan Right for You?
You may have heard friends praise their plan while seeing commercials that raise concerns. It’s easy to feel confused and wonder, “Are these plans a bad deal?” The honest answer is that there is no single “best” choice-only what is best for you. The key is to match a plan’s features with your personal health needs, budget, and lifestyle.
Let’s walk through the common praises and criticisms of medicare advantage plans to help you find clarity and confidence in your decision.
The Advantages: Why People Choose These Plans
For millions of Americans, the appeal of an Advantage plan comes down to simplicity, savings, and valuable perks. Here are the most common reasons people enroll:
- All-in-One Convenience: These plans bundle your hospital (Part A), medical (Part B), and usually your prescription drug (Part D) coverage into a single, easy-to-manage plan. One card, one company, one point of contact.
- Lower Monthly Premiums: Many plans offer low or even $0 monthly premiums. You still have to pay your standard Medicare Part B premium, but the additional plan cost can be very affordable.
- A Financial Safety Net: Every Advantage plan includes an annual maximum out-of-pocket (MOOP) limit. This is a critical protection that Original Medicare doesn’t have, shielding you from overwhelming medical bills in a tough year.
- Valuable Extra Benefits: Most plans include coverage for routine dental, vision, and hearing care-benefits not covered by Original Medicare. Many also offer fitness programs, over-the-counter allowances, and transportation to medical appointments.
The Disadvantages: Potential Drawbacks to Consider
While the benefits are appealing, it’s just as important to understand the potential trade-offs. These plans operate with certain rules that may not fit everyone’s needs:
- Network Restrictions: Most plans require you to use a specific network of doctors, specialists, and hospitals (like an HMO or PPO). Going out-of-network can result in much higher costs or no coverage at all, except in emergencies.
- Referrals and Prior Authorizations: You may need a referral from your primary care physician to see a specialist. Additionally, the plan may require prior authorization (pre-approval) before it will cover certain tests, procedures, or medications.
- Limited Coverage for Travelers: Your plan’s network is typically based in your local service area. If you travel frequently within the U.S., your coverage may be limited to emergencies only when you are outside that area.
- Annual Changes: Benefits, provider networks, and costs can-and often do-change every single year. This makes it essential to review your plan annually to ensure it still meets your needs.
Deciding between the predictable costs and extra benefits of an Advantage Plan versus the freedom of choice in Original Medicare is a deeply personal choice. Understanding these pros and cons is the first step toward making that choice with total confidence.
How to Choose Your Plan: A Simple 5-Step Checklist
Understanding what medicare advantage plans offer is the first step. Now, it’s time to take action. The sheer number of options can feel overwhelming, but this simple checklist will cut through the noise. Follow these five steps to move from confusion to confidence and find a plan that truly works for you.
Step 1: List Your Health Needs and Priorities
Before you look at any plans, first look at your own needs. A plan is only as good as how well it fits your life. Grab a pen and paper and make a few simple lists:
- Your Providers: List the doctors, specialists, and hospitals you want to keep.
- Your Prescriptions: Write down the exact name and dosage of every medication you take.
- Your Health: Are you managing chronic conditions or are you generally healthy?
- Your Wish List:: What extra benefits matter most? Rank things like dental, vision, hearing, or fitness programs.
Step 2: Compare Plans in Your Local Area
Plans are specific to your county or zip code, so a plan your friend loves in another state may not be available to you. Start by using the official Medicare Plan Finder tool to see what’s offered in your area. Look beyond the monthly premium and check the plan’s total potential costs, including deductibles, copays, and especially the Maximum Out-of-Pocket (MOOP). Also, look for the plan’s CMS Star Rating, a key indicator of quality and member satisfaction.
Step 3: Verify Your Doctors and Drugs Are Covered
This step is absolutely critical. Never assume your doctors or drugs are covered. For every plan you consider, check the provider directory to make sure your doctors are in-network. Then, call your doctor’s office directly to confirm they accept that specific plan. Next, check the plan’s drug formulary (its list of covered drugs) to ensure your medications are included and to see what they will cost.
Step 4: Understand the Network Rules
Does the plan require you to use a specific network of doctors (like an HMO), or does it offer more flexibility to see out-of-network providers (like a PPO)? Understanding these rules is key to avoiding surprise bills and ensuring you can get care where and when you need it.
Step 5: Get Unbiased Guidance to Finalize Your Choice
You’ve done the research, but how can you be sure you’ve made the right choice? This is where expert guidance provides peace of mind. Feeling stuck? The Modern Medicare Agency can walk you through these steps, double-check your work, and help you steer clear of costly enrollment mistakes. We provide clear, unbiased advice so you can enroll with complete confidence.
Key Enrollment Periods: When You Can Join or Switch Plans
One of the most common points of confusion with Medicare is that you can’t just sign up or change your plan whenever you want. Enrollment is limited to specific times of the year, and missing these deadlines can unfortunately lead to late enrollment penalties or long gaps in your coverage. Understanding these key dates is the first step toward gaining confidence and control over your healthcare.
Let’s break down the calendar into simple, easy-to-remember periods.
Your Initial Enrollment Period (IEP)
This is your first and most important window to sign up for Medicare. Your IEP is a 7-month period that starts 3 months before the month you turn 65, includes your birthday month, and ends 3 months after. For example, if your birthday is in June, your IEP runs from March 1 to September 30. Enrolling during this time helps you avoid lifelong penalties.
Annual Enrollment Period (AEP)
Often called “Fall Open Enrollment,” this is the time for most people who are already enrolled in Medicare to make changes. From October 15 to December 7 each year, you can switch between medicare advantage plans, move from an Advantage Plan back to Original Medicare, or join a Part D prescription drug plan. Any changes you make will take effect on January 1 of the following year.
Special Enrollment Periods (SEPs)
Life is unpredictable, and certain events may allow you to change your coverage outside of the standard enrollment periods. These qualifying life events trigger a Special Enrollment Period. Common examples include:
- Moving to a new address that isn’t in your current plan’s service area.
- Losing other health coverage (like from an employer).
- Your plan changes its contract with Medicare.
- You qualify for Extra Help to pay for prescriptions.
Navigating these dates can feel overwhelming, but you don’t have to do it alone. Ensuring you enroll at the right time is critical to protecting your health and your finances. If you’re unsure which period applies to you, getting simple, trusted guidance can help you move from confusion to confidence.
From Confusion to Confidence: Your Next Step in Medicare
Navigating your healthcare options can feel overwhelming, but understanding the fundamentals is the first step toward peace of mind. We’ve seen that medicare advantage plans offer an all-in-one alternative to Original Medicare, but the right choice depends entirely on your personal health needs, budget, and preferred doctors. Remembering the key differences between plan types and being mindful of enrollment periods are crucial for avoiding costly mistakes and coverage gaps.
You don’t have to make this critical decision alone. As a licensed, independent broker with The Modern Medicare Agency, my only goal is to provide simple, unbiased guidance. I’ll help you compare options from over 40 top-rated insurance carriers to find a plan tailored to your unique needs. My advice is always personalized-never rushed, never pressured.
Take the next step toward clarity and security. Schedule your free, unbiased Medicare review with Paul today. Let’s work together to ensure you have the coverage and confidence you deserve for the years ahead.
Frequently Asked Questions About Medicare Advantage Plans
What is the biggest disadvantage of a Medicare Advantage plan?
The most significant challenge for many people is the network restrictions. Unlike Original Medicare, which allows you to see almost any doctor nationwide, an Advantage Plan requires you to use doctors and hospitals within its specific network. Going out-of-network for routine care can be very expensive or may not be covered at all. This is a crucial trade-off to consider for the plan’s lower costs and extra benefits.
Do you still have to pay your Medicare Part B premium with an Advantage Plan?
Yes, this is a critical point that often causes confusion. You must continue to pay your monthly Medicare Part B premium to the government. A Medicare Advantage Plan (Part C) replaces how you receive your Part A and Part B benefits, but it does not replace your financial obligation for Part B. Keeping your Part B enrollment current is essential to maintain your Advantage Plan coverage and avoid penalties.
Can I switch from my Medicare Advantage Plan back to Original Medicare?
Yes, you have the option to switch, but only during specific times of the year. You can leave your Advantage Plan and return to Original Medicare during the Annual Enrollment Period (October 15 to December 7) or the Medicare Advantage Open Enrollment Period (January 1 to March 31). Understanding these windows is key to making sure you have the flexibility to change your coverage if your needs evolve.
What is the annual out-of-pocket maximum (MOOP) and why is it important?
The out-of-pocket maximum is a vital financial safety net built into every Medicare Advantage Plan. It’s the most you will have to pay for covered medical services in a calendar year. Once you reach this limit, your plan pays 100% of the costs for the rest of the year. This protects you from catastrophic medical bills, a protection that Original Medicare does not offer on its own without a supplemental policy.
Are all Medicare Advantage plans the same?
No, not at all. In fact, they can be very different from one another. All Medicare Advantage plans must cover at least what Original Medicare covers, but they vary widely in their monthly premiums, provider networks (HMO vs. PPO), copays, and extra benefits like dental, vision, or hearing. This is why comparing plans carefully is so important to find the one that truly fits your personal health and budget needs.
How do I know if my doctor accepts a specific Medicare Advantage plan?
The most reliable method is to call your doctor’s office directly. Ask the billing specialist, “Are you in-network for [Specific Plan Name and Company]?” While you can also check the plan’s online provider directory, these lists can sometimes be outdated. A direct call to your trusted provider is the best way to get a clear, confident answer and avoid any unwelcome surprises when you need care.
What happens if I need care while traveling outside my plan’s service area?
You are always covered for emergency and urgent care anywhere in the United States. However, for routine, non-emergency care, you are typically required to see providers within your plan’s specific service area. Some PPO plans may offer partial coverage for out-of-network routine care, but your costs will be higher. It’s important to understand your plan’s rules for travel before you go, giving you peace of mind on your trip.






